The Life Cycle of a Drug
You’re reading a free article with opinions that may differ from The Motley Fool’s Premium Investing Services. Become a Motley Fool member today to get instant access to our top analyst recommendations, in-depth research, investing resources, and more. Learn More
Here's a wee bit of trivia to stump and amaze your friends, something I learned just the other day at Fool HQ. What was the law they were trying to pass in "I'm Just a Bill"? (Answer at the end of the column.)
That song introduced many of us to the torturous process required to turn a good idea (I'm generalizing here) into a law. I am to this day thankful that the song remained at a high enough level that they didn't delve too deeply into Robert's Rules of Order for lyric ideas. I mean, what rhymes with "point of parliamentary procedure" or "filibuster"?
Ham-handed segue warning.>
I am enough of a cynic that although I do not believe the laws that end up passing are, ahem, much improved by the process, the U.S. political cycle does have the benefit of keeping lawmakers from screwing up too much. The process, therefore, benefits us by filtering out most of the truly bad ideas.
Moving drugs from concept to market works much the same way, with the added factor that, unlike most laws, drugs have a defined ending date, delimited by the patent expiration. (I would welcome this in the U.S. legal system, by the way.) En route, most drugs are eliminated due to issues of efficacy, side effects, obsolescence, commercial viability, or regulatory scrutiny. The process can be grossly expensive, but it serves the purpose of self-selecting only the most effective pharmaceutical products for release to the general public.
I'm speaking about this as a Rule Maker feature in deference to our holdings in Pfizer (NYSE: PFE) and Schering-Plough (NYSE: SGP). Last Monday, I wrote about the importance of effective deployment of research and development (R&D) resources as a way of determining if a company's management is adding value. Several readers correctly pointed out that one of the difficulties of doing this -- with pharmaceutical companies in particular -- is that deployed R&D oftentimes does not provide any return for more than 10 years, so it is somewhat deceptive to compare current R&D with current returns.
A very good point. So I've spent some time over the past week getting a better understanding of the drug life cycle. I now understand how little I actually know on the subject, a fact that I will soon prove to the more experienced pharmaceutical hands out there. But not to worry, this is what Foolishness is all about. I'm certain that someone out there will learn something from my exercise in learning, just as others will further guide me in my own understanding.
So with that in mind, I am going to blatantly plagiarize one of the Pfizer message board contributors. In September, VaLurch put together a brief description of the drug approval process as part of an absolutely excellent FAQ on the company. I could not describe it better than he, a medical technologist, has done for us, so I will simply italicize any additional comments I have on the subject.
The Drug Approval Process
It takes an average of 12-15 years for a new drug to come to market. There are pathways that can speed the approval process (called fast-tracking) for certain diseases like cancer and AIDS. Only one of every thousand compounds evaluated makes it to human testing and only one of every five drugs gets approved. The Food and Drug Administration (FDA) oversees the approval process in the United States.
A few things to note here. First of all, these four sentences should drive home how crucial proper control of R&D is to drug companies. For one, except for fast-tracked drugs (jtrudel, also of the Pfizer board, has an excellent description of this process in the FAQ), any developed compound will take up to 12 years to return a dime, and the vast majority of these efforts never produce any revenue at all. The key is how a company manages its R&D, for early elimination of compounds from further study would GREATLY reduce the drag of non-returning investments. Given the percentages, the company that best uses reinvested capital is the one that allocates its resources to the drugs most likely to be approved.
Preclinical Testing
A pharmaceutical company will conduct laboratory and animal studies to determine the effects of the potential drug on the targeted disease. The safety of the compound must also be evaluated. This process usually takes three-and-a-half to six years.
At this point a company patents the drug. U.S. patents are good for 20 years and are not extended to the point of commercial gain, meaning that an 11-year approval process eats up 55% of the time a company has exclusive use of a drug.
Investigational New Drug Application (IND)
If the preclinical testing shows promising results, the pharmaceutical company will apply to the FDA for an Investigational New Drug Application. The IND must include the chemical structure of the drug; how it works in the body; the results of the preclinical testing, including any toxic side effects; how, where, and by whom the human studies would be performed; and how the drug will be manufactured. The IND becomes effective if the FDA does not deny it within 30 days.
Phase I Clinical Trials
Phase I studies usually involve 20-80 healthy volunteers (sometimes paid for participation). This phase is designed to test for safety by determining what happens to the drug in the human body -- how it is absorbed, metabolized (processed in the body), and excreted. A safe dosage range is determined by measuring the duration of the drug's intended effect and investigating side effects as the dosage is increased. Phase I trials usually take several months to a year. About 70% of drugs pass this testing.
Phase II Clinical Trials
Phase II studies usually involve 100 to 300 volunteer patients. This phase is designed to test for efficacy (i.e., does what the drug is supposed to do -- cure the disease or lessen the symptoms). Most Phase II studies are randomized trials. The patients are divided into groups: one to receive the experimental drug, one to receive a placebo, and sometimes one to receive the standard treatment. Often, to minimize bias, a double-blind study is done, meaning that neither the patients nor the doctors running the trial know which patients are assigned to which group. The study should yield information about the safety and effectiveness of the new drug. Phase II testing may last from several months to two years. About one-third of the experimental drugs tested complete Phase I and II studies.
At this stage, the company also works on proper dosage for the drug.
Phase III Clinical Trials
Phase III studies usually involve 1000-3000 patients in clinics and hospitals. These large clinical trials are designed to prove conclusively that the drug works better than the standard treatment for the disease in question. Most Phase III studies are randomized and double-blind. All of the patients are asked to list any side effects that occur while they are in the study. Phase III testing usually takes around three years and approximately 80% of the drugs that enter this phase successfully complete the testing.
A study involving such a long period of time and so many people is extremely costly. Pharmaceutical companies are better off abandoning drugs with marginal efficacy or a high indication of side effects during Phase II than to endure the expense of Phase III trials. The resources required is one reason why I believe that the debate of high gross margins on drugs is completely misplaced, as it misses the point that the majority of the cost basis on a drug is not derived from production. Rather, a drug company's cost structure must be designed to allow a sufficient return on investment both for the R&D for that individual property and the non-returning "impaired assets" that have no chance of equitable return. For this reason I believe that price controls on drugs would be disastrous for American healthcare, as drug companies would no longer have the incentive to concentrate on development of new cures.
Phase III is where much of the "quality of life" types of questions are answered, such as whether a treatment can help people live longer. These types of concerns are known as "surrogate endpoints."
New Drug Application (NDA)
Once the phase III clinical trials are completed, the drug manufacturer compiles and analyzes all the data. If the data demonstrates the safety and effectiveness of the drug, an NDA is filed with the FDA. The average review time for an NDA is two-and-a-half years. FDA approval gives the manufacturer the right to market the drug exclusively under a trademark name for the time remaining on the patent of the drug. When the patent expires, other manufacturers may produce the drug in generic form or under a different brand name.
It was at this point that Schering-Plough's Vasomax (co-marketed with Zonagen) was withdrawn this past June, when it became clear that the FDA would not approve it. This is the worst-case scenario for a drug company, when they have maximized their expenditures upon an asset that will not provide any return. Schering-Plough and Zonagen (Nasdaq: ZONA) have reported that they intend to re-submit Vasomax (an erectile dysfunction treatment) after clinical refinements.
Phase IV Studies
Phase IV studies are any additional collection of data from patients after the drug has received FDA approval. Patients may have a checklist to mark off or may be asked to report any other symptoms or side effects.
Phase IV studies, for example, were responsible for Schering-Plough's reapplication for Claritin to be labeled for treatment of seasonal allergies. The drug was initially indicated as a dermatology treatment. In receiving the approval, Schering-Plough was able to re-patent Claritin and receive an additional 20 years of exclusive use for its use for allergies.
Recalls/Restrictions
Occasionally, when a drug becomes available and thousands of new patients begin taking the drug, an unexpected severe reaction or side effect may appear that was not detected with the smaller test groups in the clinical trials. The reaction must be deemed excessive by the FDA compared to the drug's benefits or other drugs/treatments available for a drug to be recalled. Often, restrictions will be placed upon the circumstances for which the drug may be prescribed.
Some infamous recalls in recent years have been Wyeth-Ayerst's Fen/Phen (restricted once a link to severe cardiovascular disease was made) and Pfizer's Trovan (found to have caused several deaths from certain liver disorders). In neither case was the drug completely withdrawn from the market; rather, the FDA forced the companies to re-label the drugs to limit their use in cases where a high risk of side effects are possible.
In the case of Trovan, a newly released drug will now be made available only to a fraction of the cases for which years of trials had shown it to be effective. This affirms a point that should not be overlooked in regard to pharmaceuticals: For better or worse, the science of developing drugs is never exact. Scientific method is constantly refining how certain treatments are used, and will continue to do so.
And finally, the answer to the Schoolhouse Rock trivia question: They wanted to require school buses to stop at railroad crossings. Now you have something to stump your friends with. Just make sure not to ask one of the other six people who read my entire column.
Viva la Fool!
Invest Smarter with The Motley Fool
Join Over Half a Million Premium Members Receiving…
- New Stock Picks Each Month
- Detailed Analysis of Companies
- Model Portfolios
- Live Streaming During Market Hours
- And Much More
Motley Fool Investing Philosophy
- #1 Buy 25+ Companies
- #2 Hold Stocks for 5+ Years
- #3 Add New Savings Regularly
- #4 Hold Through Market Volatility
- #5 Let Winners Run
- #6 Target Long-Term Returns
Why do we invest this way? Learn More
Related Articles





Motley Fool Returns

Market-beating stocks from our award-winning analyst team.
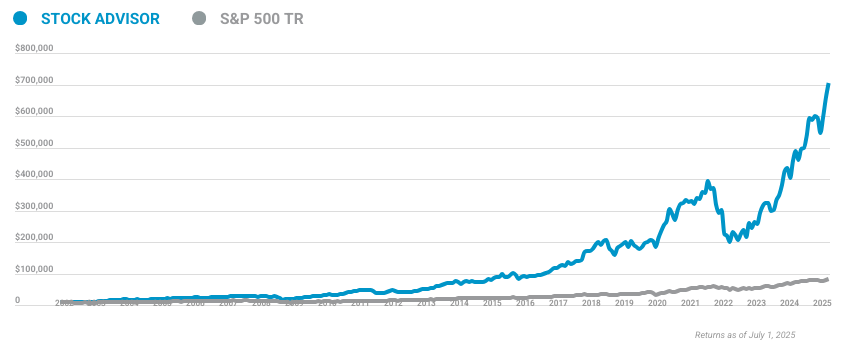
Calculated by average return of all stock recommendations since inception of the Stock Advisor service in February of 2002. Returns as of 04/17/2024.
Discounted offers are only available to new members. Stock Advisor list price is $199 per year.
Calculated by Time-Weighted Return since 2002. Volatility profiles based on trailing-three-year calculations of the standard deviation of service investment returns.
Premium Investing Services
Invest better with The Motley Fool. Get stock recommendations, portfolio guidance, and more from The Motley Fool's premium services.