Image source: The Motley Fool.
Fresenius Medical Care AG & Co. KGaA (FMS -0.28%)
Q4 2020 Earnings Call
Feb 23, 2021, 9:30 a.m. ET
Contents:
- Prepared Remarks
- Questions and Answers
- Call Participants
Prepared Remarks:
Operator
Ladies and gentlemen, thank you for standing by. My name is Emma, your Chorus Call operator. Welcome and thank you for joining the Fresenius Medical Care Earnings Call on the First -- Fourth Quarter and Full-Year 2020 Results. [Operator Instructions] The presentation will be followed by a question-and-answer session. [Operator Instructions]
And I would now like to turn the conference over to Dominik, Head of Investor Relations. Please go ahead, sir.
10 stocks we like better than Fresenius Medical Care
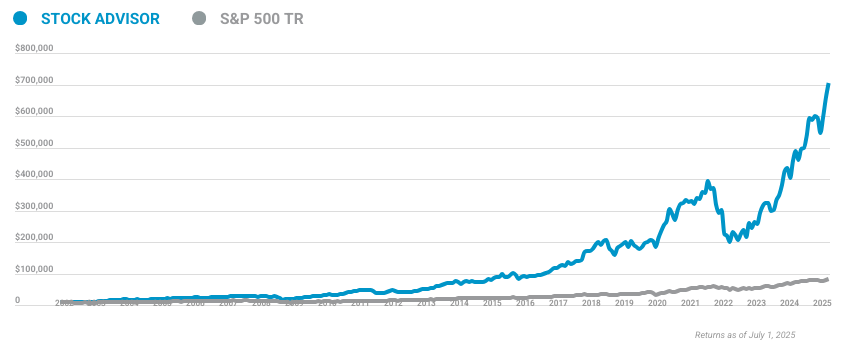
When investing geniuses David and Tom Gardner have a stock tip, it can pay to listen. After all, the newsletter they have run for over a decade, Motley Fool Stock Advisor, has tripled the market.*
David and Tom just revealed what they believe are the ten best stocks for investors to buy right now... and Fresenius Medical Care wasn't one of them! That's right -- they think these 10 stocks are even better buys.
*Stock Advisor returns as of November 20, 2020
Dominik Heger -- Executive Vice President, Head of Investor Relations, Strategic Development & Communications
Thank you, Emma. As mentioned by Emma, we would like to welcome you to the Fresenius Medical Care earnings call for the fourth quarter and full year 2020. We appreciate you joining today to discuss more details following our early indications call at the beginning of the month.
Now, it is my pleasure, as always to start out the call by mentioning our cautionary language that is in our Safe Harbor statement, as well as in our presentation and in all the marketing material that we have distributed earlier today. For further details concerning risks and uncertainties, please refer to these documents as well as to our SEC filings. I do assume that there are numerous questions this time. Therefore, we have reserved 90 minutes for that call, but would like to limit the number of questions again to two in order to give everyone the chance to ask questions. Should there be further questions and time left, we can go a second round. It would be great, if we could make this work again.
With us today is, of course, Rice Powell, our CEO and Chairman of the Management Board. Rice will give you some more color around the strategy and business development. He will be joined by Frank Maddux, our Global Chief Medical Officer, who will provide a medical update with a focus on COVID-19. And of course, also with us is Helen Giza, our Chief Financial Officer, who will give you a detailed update on the financials, as well as our targets for 2021 and 2025.
I will now hand over to Rice. The floor is yours.
Rice Powell -- Chief Executive Officer and Chairman
Thank you, Dominik. Hello, everyone. Thank you for joining our presentation and for your continued interest in Fresenius Medical Care. I'll begin my remarks on Slide 4. At Fresenius Medical Care, we have a common purpose, which is creating a future worth living for patients worldwide every day and this purpose that unites our team was never more evident than throughout 2020. In the face of unprecedented COVID-19 pandemic, we delivered life-sustaining dialysis treatments to nearly 347,000 patients and over 4,000 clinics worldwide. The number of treatments we provided increased by 3% to slightly over 53 million treatments, and we did all of this with uncompromising focus on our quality of care.
Before we go any further, it's important for me to take a moment to once again say thank you to our employees around the world for their tireless efforts and relentless focus on patient care during these extraordinary times. This is a remarkable achievement. I would also like to acknowledge our patients that sadly passed away and acknowledge everyone that's grieving from the loss of a loved one during this terrible pandemic. Our thoughts are with you during this very painful time.
Moving to Slide 5. This pandemic has not changed the fact that the number of patients facing advanced kidney disease and requiring dialysis on a global basis is projected to grow after the effects of the pandemic has annualized out. There are several factors contributing to this.
One, people around the world are simply living longer. By 2030, the number of people over age 65 is expected to increase significantly to around 1 billion people globally. Two, hypertension, already one out of every four adults around the world suffers from high blood pressure. And lastly, diabetes, by 2030, the number of patients with diabetes is anticipated to grow to more than 0.5 billion. Considering these trends, we continue to project that over 6 million patients will need regular dialysis by 2030. We recognize our responsibility to this patient population and believe that we are well positioned to continue to address this growing need.
This leads to our strategy on Slide 6. At our Capital Markets Day last October, we introduced our 2025 strategy. Now more than ever, we feel that this is the appropriate strategy as it prioritizes patients' needs and quality of care aligned with key drivers and developments for our industry and positions our business to deliver sustainable growth over the medium term and beyond.
The first leg and core of our strategy focuses on the renal care continuum. We know that the patient population with advanced renal disease around the world continues to grow. We also know that these patients will encounter different phases of care and modalities for treatment. It is our goal to be able to provide holistic care for our patients throughout their complete treatment path or what we are calling the Renal Care Continuum.
Building on our global vertically integrated business model, the Renal Care Continuum brings together both dialysis products and services, and features four main components, new renal care models where we will apply digital technologies such as artificial intelligence and the capability to analyze huge amounts of data. This also captures our push toward increasing home dialysis treatments.
In value-based care, we already lead the way in transitioning from the historic fee-for-service payment model to pay-for-performance models in order to provide superior care, while ensuring it remains affordable. Our Humana contract is a perfect example of how we are already moving forward in this regard. With chronic kidney disease and transplantation, we are expanding beyond dialysis to the treatment of CKD and also looking to play an active role in the area of kidney transplantation. And with renal care innovations, we aim to be at the forefront of any industry disruption by developing our own renal care innovations as well as investing in start-ups and early stage companies in our space.
Critical Care solutions is the second leg of our strategy. Here, we seek to further extend our critical care portfolio to other extracorporeal intensive care therapy areas, such as treatment of heart, lungs and multi-organ failure. Finally, complementary assets makes up the third and final leg of our strategy. Our goal here is to continue to expand our network of complementary assets through partnerships, investments and acquisitions. These assets will help us, for example, to coordinate patients efficiently and thereby, add value in two dimensions in terms of creating medical value and in managing patient-related costs.
I want to reiterate that COVID-19 has not altered our strategic view. We are committed to executing on this strategy in delivering on our 2025 targets. When we announced our strategic plan for 2025, we had not included COVID-19 as a negative effect. However, as the effects from the pandemic accelerated at the end of 2020, its impact became significantly more pronounced. We strive to compensate for the anticipated negative COVID-19 effects on our 2025 targets by transforming our global operating model and reducing our cost base sustainably, while we execute on our 2025 strategy. We will touch on this more in the presentation.
Turning to Slide 7. We are proud of the positive impact our life-sustaining products and services have on key patients we treat. As a large global organization, we also recognize our responsibility for the broader impact we have on the environment and on society throughout the world.
I'm pleased to report that despite the challenging environment we faced in 2020, we have made real progress on our sustainability journey. Last year, we launched our global sustainability program to step up and drive the integration of sustainability into our business practices worldwide over the course of the next three years from 2020 to 2022. The program, which is under my direct responsibility, establishes common goals, responsibilities and key performance indicators.
During 2020, we introduced ESG targets for management compensation that are directly linked to the progress of our global sustainability program, further underscoring the program's importance. In the last year, we defined global standards for how we measure our patients' feedback. We approved a new policy around human and labor rights, and we rolled out a global code of conduct for our suppliers.
We believe that we need good data to understand our impact and decide on global goals in the future. This is why we implemented several new global KPIs for sustainable development. Going forward, we will measure progress with performance indicators for topics such as quality of products and care as well as responsible business practices. The feedback we received from our stakeholders and their interest in our sustainability activities are also very important to us.
We want to be transparent about what we strive to achieve and how we are progressing. This is why we will report on our progress and align with international standards such as those of the Sustainability Accounting Standards Board and the recommendations of task force on climate-related financial disclosure. In our upcoming non-financial report, we have included more than 100 KPIs that will speak to this commitment.
With that, it's my pleasure to now hand over to Frank for his medical update.
Franklin W. Maddux -- Global Chief Medical Officer
Thank you Rice, and I appreciate the chance to speak today in somewhat more detail than I was able to at the early indications call we had on February 3. I wish to provide you with some perspective on the clinical burden we have experienced from COVID, as well as the impact and outlook. I will comment on mitigating factors we are analyzing in the patients we treat both directly and indirectly around the world.
As a reminder, the pandemic is the result of a highly contagious virus that causes severe respiratory distressed syndrome and a substantive inflammatory response that can lead to a multi-organ failure and long-term sequelae. This virus has changed over the course of 2020, and now in 2021, we see variations in the genetic makeup of the virus. It is these mutations of the virus that make the outlook for our patients, one which will continue to be dynamic until our general population has developed immunity and we learn if immunity is conferred to these variants.
Infectious disease experts note 70% to 85% of the general population need significant immunity to achieve notable reductions in the pandemic risk that causes disruptions to our healthcare systems and economies.
Moving to Slide 9, we see the global accumulation of COVID infections over the course of 2020 and into 2021. These surges were at first isolated to specific countries and regions around the globe, but as the pandemic progressed through the year, we observed a remarkably broad-based infection profile emerge. In late 2020, the surge in cases was multinational and broad-based throughout affected geographies with peak infections occurring in December and Europe and in mid-January in the United States. The experience of the general population is mirrored in the exposure in cases documented in our own end-stage kidney disease patients. We have seen the case rates for COVID at Fresenius Medical Care grow through the early weeks of 2021.
COVID was correlated with local clinical realities that we had to adapt to. Each country managed the pandemic slightly differently. By example, throughout much of Europe when a dialysis patient became COVID positive, they were referred to a government healthcare location for isolation treatment, while patients free of disease were transferred into our facilities. This provided support of our prevalent patient count until the large late year European wave began and fewer patients were available to reenter the system.
In other countries, like in the United States, dialysis clinics had to set up and run a network of isolation clinics or shifts to treat COVID positive or suspected people. At its peak on January 17th, we operated 621 isolation locations spread across the country. As these COVID surges have peaked, hospital and healthcare facilities began to limit non-COVID care. This was a distinct strain on our population of patients who have a higher proportion of diabetes, cardiovascular disease, and other conditions requiring ongoing clinical care.
The progression of Fresenius Medical Care exposure to the virus and the depiction of the waves that were observed correlates with the curves seen in the general population both globally and regionally. The latest wave has been during the winter months for the Northern Hemisphere countries and reached a peak in January of this year. Despite the most recent weeks of decline in cases, there has been a concomitant increase in the number of locations that have outbreaks with the newer variant strains identified as the UK and South African variants.
Moving on to Slide 10, our reported key clinical indicators highlight the stability of clinical results in our patients receiving their routine treatments. You will note the slightly lower general hospitalization days seen in several regions that has been seen throughout the pandemic as routine care patterns were disrupted. We saw stable anemia as well as bone and mineral metabolism control demonstrating that our patients are continuing to receive highly reliable dialysis care.
Moving on to Slide 11. On this slide, I wish to address the phasing we noted during the early indications call in the excess death rate compared to our baseline. These data show the delta to the normative values as we analyze the full year against known seasonal variability.
I will reiterate my comment from February 3rd. The capturing all deaths due to COVID trails by four to five weeks due to the nature of the illness and the fact that reporting became progressively delayed as identified cases were treated more intensively as the year progressed, but not within our own walls.
I would note that as an acute COVID surge occurred in the general population, we observed a higher-than-normal incidence of acute kidney injury and increased need for critical kidney disease care. When observing this added care, combined with the reduced treatments due to the COVID-related excess deaths, we feel the dominant effect in the loss of patients that would have been expected to dialyze in the coming months is impacting the outlook.
The impact we have seen in North America moving on to Slide 12 and EMEA is that across all age groups COVID has generated excess deaths and is not confined only to the elderly or diabetic populations. It is notable that excess deaths have not led to a change yet in these base-level population demographics of our patients.
Excess death due to COVID is not confined to Fresenius Medical Care, nor only to people with end-stage kidney disease. It is now reported across the globe as the general population has seen an excess death rate that mirrors what we are seeing in the population of CKD and end-stage kidney disease patients. These findings underpin our cautions around projections for the year despite a rebound in referrals as health systems and doctors address the need for usual care to resume.
Going on to my final Slide 13, we are reminded that immunity from vaccination is about not just vaccinating our population of patients and staff, but developing community immunity. Fresenius Medical Care is developing experience with almost all of the approved vaccines across the world and is attempting in a number of countries to have the dialysis facility become a point of distribution and delivery of these vaccines to patients and staff.
Getting to herd immunity at the levels recommended in the communities we operate, where 70% to 85% of people need antibodies to COVID will be challenging. We have active campaigns to address questions about the vaccine. Understand the immunity vaccination confers on our dialysis patient and address the vaccine hesitancy that is slowing the ability to put the pandemic in the rearview mirror.
Our expectation of the future is that some effects of the pandemic will be with us through a significant portion of 2021 and possibly beyond. We hope that vaccination, persistent attention to non-pharmaceutical interventions, active surveillance for COVID cases, and active treatment of new cases will begin to turn the tide on the excess deaths and return results to our expected norms in the second half of 2021. We do not see data to date that leads us to believe that the return will be below expected norms. This return to normalcy will afford the chance to begin to work on numerous active clinical initiatives to protect the cardiovascular system of our patients and begin to target the next level of achievement in patient outcomes.
With that, I will turn it back to Rice.
Rice Powell -- Chief Executive Officer and Chairman
Thank you, Frank. I'll continue my remarks beginning on Slide 15. Despite COVID-19, we achieved our revenue target for 2020 and overachieved on net income for the year, and thus setting ourselves a higher performance bar for 2021 than we had originally planned. As we indicated earlier this month, there are two significant developments impacting our developments in the fourth quarter of 2020.
Number one is the EUR195 million goodwill impairment in our Latin American segment. The impairment was driven by macroeconomic downturn and increasing risk adjustment rates for certain countries in the Latin American region.
Secondly, the impact in the fourth quarter relates to the excess mortality of dialysis patients that accelerated in the US and in EMEA in November and December in particular and accumulated to approximately 10,000 patients over the pre-pandemic baseline. This is an effect that will continue to impact our business in 2021.
2020 was a positive year for growth in home dialysis. We reached 14% of treatments in the United States in a home setting. This implies a 13% increase in the number of home treatments compared to 2019, with home hemodialysis growing around of 37% and peritoneal dialysis contributing a solid 7% growth in the US. We are well on track to achieving our 2022 target of having 15% plus of dialysis treatments in the United States in a home setting. On the basis of our strong business performance during 2020, we plan to propose a dividend increase at our Annual General Meeting in May.
Turning to Slide 16. During the fourth quarter, we achieved revenue of $4.4 billion, particularly in the United States -- I'm sorry, $4.4 billion reflecting 4% growth in constant currency. As mentioned earlier, the impact of accelerated excess mortality, particularly in the US and EMEA, had a negative impact on our growth.
On an adjusted basis, excluding the EUR195 million goodwill impairment in Latin America, our operating income grew 5% in constant currency and our net income grew 6% in constant currency for the fourth quarter. One of the larger contributors was a negative prior year revenue recognition adjustment related to accounts receivable.
COVID-19-related costs, such as elevated prices for personal protective equipment and higher compensation for our frontline workers, especially those in isolation clinics weighed heavily on the earnings for the quarter. Our business also faced substantial headwinds from foreign currency translation effects in all regions during the fourth quarter.
Turning to Slide 17. Even with all the challenges of COVID-19 for the full year, we achieved 5% revenue growth at constant currency, in line with our stated target achievement -- stated targets for 2020. Our services business delivered 2% same-store growth and had a very strong year boosted by products for acute care treatments and home dialysis products.
Our full year net income growth exceeded our guidance range with 12% growth in constant currency. While we are proud of this outperformance in 2020 in net income growth, it consequently raised the bar by around 300 basis points against our plan for '21. Additionally, the recent negative foreign exchange rate effect presents a significant headwind right from the beginning of the year, almost bringing net income growth to flat for 2021, excluding the negative impact from COVID.
Turning to Slide 18. Given our earnings growth in 2020 and in line with our dividend policy, we plan to propose a 12% dividend increase to EUR1.34 at our Annual General Meeting in May of this year. If approved, the proposal will result in our 24th consecutive dividend increase and an annual dividend growth CAGR of 10.9% over the last five years. We believe in the underlying strength of our business model despite the challenges that have presented themselves via COVID-19.
Looking to Slide 19. Besides the high base we have created in 2020 and the mentioned sizable headwinds from exchange rates, we anticipate several important tailwinds for our business during 2021. These include the expansion of value-based care programs as the industry transitions away from the fee-for-service payment model, improved reimbursement rates given the gradual shift of patients from Medicare to Medicare Advantage plans, the continued trend toward dialysis treatments at home, and the positive effects from the completion of cost optimization measures that are coming to fruition.
While these tailwinds do not offset the significant headwinds we are facing in the short term, the progress in these areas has positive implications for the strength of our business as we look out to the medium and longer term. For 2021, COVID-19 remains the dominant theme, and we are expecting the headwinds to be significant. The excess mortality of dialysis patients due to COVID-19 has an ongoing effect on treatment volumes and will take until 2022 to annualize out.
With lower treatment volumes, we also see lower clinic utilization also downstream -- other downstream assets. This also reduces our ability to absorb wage inflation and fixed cost inflation. This impact is also pronounced in EMEA where excess mortality has been high and the workforce is generally less flexible in terms of reallocating shifts. We anticipate the increased need and higher costs for personal protective equipment to remain with us as well as higher pay for employees working in our special isolation clinics.
During 2020, we had significant SG&A savings, for example, from less travel and meetings and self-insured health plans in the United States. While this contributed to positive net income performance in 2020, we do expect these trends to partially reverse in the second half of 2021, but with spending remaining below the 2019 levels. Beyond COVID-19, we see negative headwinds from calcimimetics reimbursement and anticipate transactional exchange rate losses.
While 2021 has the makings of a challenging year, we remain optimistic about our future and are focused on executing our 2025 strategy and achieving our corresponding financial targets. Therefore, in the year of our 25th anniversary as a company, we plan to transform our global operating model to sustainably reduce our cost base and to put us in good standing for the next 25 years. We are referring to this program as FME25 and Helen will touch on it in more detail at the end of her remarks.
And with that, it's my pleasure to turn the meeting over to Helen.
Helen Giza -- Chief Financial Officer
Thank you, Rice. Hello, everyone. I will begin on Slide 21, which illustrates our target achievements during 2020. And coming with the earlier comments, I am very proud of the results we delivered in 2020, achieving revenue growth in line with our guidance and over achieving on our net income target, all while facing an unprecedented pandemic.
On a constant-currency basis, we achieved EUR18.4 billion in revenue, a 5% increase from 2019. This includes over EUR1 billion in business growth hampered by a negative net COVID effect of EUR174 million. You will remember that for the first nine months of 2020, we reported a net neutral impact from COVID-19, so it wasn't until the end of the fourth quarter that we really took a hit. Our reported revenue for the year includes a negative EUR536 million impact from foreign exchange rates.
On net income, again on a constant-currency basis, we achieved EUR1.4 billion, representing a 12% increase from 2019. This includes a negative net COVID effect of EUR50 million, again largely linked to developments in the fourth quarter. Reported net income for 2020 also reflects a negative translational exchange rate impact of EUR20 million as well as a EUR195 million impairment in our Latin America business as a result of macroeconomic-driven developments impacting goodwill and trade names in the region.
As we are looking ahead to 2021, the strong achievement in net income before special items set a roughly 300 basis points higher-than-planned baseline. Based on the current exchange rates, we see a significant headwind in 2021. Taking this and the unexpectedly higher base into account, net income growth for 2021 is close to flat, excluding the negative COVID-19 effect.
I will now turn to Slide 22 to look at the fourth quarter in more detail. During the fourth quarter, we achieved organic growth of 1% despite sizable headwind, thanks in large part to our global footprint. As highlighted earlier, excess mortality of dialysis patients significantly accelerated in the U.S. and in EMEA, especially in November and December. However, solid organic growth developments outside North America supported by the product business, led to positive organic growth for our business overall. All regions experienced negative foreign currency developments during the quarter.
Moving to Slide 23. Despite COVID-19, we were able to continue our organic growth, especially in the area of home dialysis. On the positive side, performance for our services business was supported by a negative prior-year revenue recognition adjustment related to accounts receivable and we also saw an improvement in reimbursements.
Treatment growth was also positive with overall same-market treatment growth of 1% worldwide during the fourth quarter. The biggest negative driver for the quarter was the loss of treatments related to accelerated excess mortality of dialysis patients in North America and EMEA. This was very pronounced in particular in December. Therefore, the impact on 2020 was rather small, while consequently the annualization effect of lower treatments for 2021 has significantly grown. The services business also faced expected headwinds from lower reimbursement from calcimimetics as well as unfavorable foreign currency translation.
I will move to the products performance on Slide 24. Our products business delivered strong growth in the fourth quarter with 8% organic growth. The remarkable 30% growth in non-dialysis products albeit representing just EUR26 million in revenue was all driven by product sales for acute or critical care treatments. Growth in dialysis products was also boosted by sales of products that support treatments in an acute setting.
The products business also benefited from higher sales of in-center disposables and the growth trend in home dialysis treatments, with higher sales of both home HD and PD products. Performance of the products business was somewhat impacted by lower sales of in-center machines for chronic treatment, and again foreign exchange rates were a negative headwind here as well.
Moving to Slide 25. Our overall Group margin decreased from 13.5% to 10.5% in 2020. The bar chart on the left shows the regional contributions and corresponding margins for the fourth quarter of 2020 compared to the fourth quarter of 2019. North America, EMEA and Asia-Pacific all saw improvements in their margin year-over-year, but not enough to make up for the margin deterioration in Latin America as a result of the EUR195 million impairment. On the positive side, the biggest margin driver during the fourth quarter was the already mentioned negative prior-year revenue recognition adjustment, but the Group margin also benefited from continued lower G&A spend, such as travel and meetings.
After the Latin America impairment, the negative effects from COVID-19 posed the greatest headwind to margin development. COVID-19-related excess mortality negatively impacted, in particular, North America and EMEA in the fourth quarter. Continued cost required to operate safely through the pandemic, including PPE and higher compensation for frontline workers and isolation clinics, also weighed on margin development. Finally, the fourth quarter margin was also negatively impacted by the anticipated lower reimbursement from calcimimetics.
Turning to Slide 26. Here, we look at the cash flow developments during the fourth quarter. In the last quarter, we generated EUR584 million of operating cash flow, resulting in a margin of 13.3%. Free cash flow for the fourth quarter totaled EUR283 million with the resultant margin of 6.4%.
When you look at the leverage ratios on the bottom left of the page, including IFRS 16, our leverage ratio decreased to a 2.9 times net debt-to-EBITDA ratio during the fourth quarter, just below our target range of 3.0 to 3.5. If we were to include the positive effect of U.S. federal relief funding and advanced payments under the CARES Act, which will reverse itself, the net debt-to-EBITDA ratio for the quarter would be at 2.7 times. The weightings presented in the bottom right box further confirm our solid financial position.
Turning to Slide 27. This brings us to our outlook for 2021. On a constant-currency basis, we are expecting revenue growth of low- to mid-single digits and a decline in net income in the high-teens to mid-20s percentage range. I would explain how we get to these ranges in a moment, but I want to be clear on some key assumptions.
We expect excess mortality to continue to accumulate through the first half of 2021. We are also assuming COVID-19-related costs in our dialysis service business, such as the provision of PPE and higher compensation for employees working in isolation clinics to remain on a high level. We are not assuming any further public relief funding beyond the already announced expansion of Medicare sequestration through March 2021. And our 2021 targets exclude special items such as the costs related to FME25, which I will comment in a minute.
Anticipating your modeling requirement for 2021, I would like to share some other relevant assumptions. We anticipate corporate cost in the range of EUR480 million to EUR500 million at constant rates. For our financial results, we expect the range of EUR340 million to EUR360 million at constant rates and we assume a tax rate of 24% to 26%.
I will now turn to Slide 28. Earlier, we highlighted the tailwinds and headwinds we are expecting to face in 2021. While we don't know exactly how the different drivers will develop over the course of the year, we have attempted to at least visualize our assumptions and provide some perspective on the scale of the various revenue and net income drivers.
I won't walk through every effect here, but not surprisingly, COVID-19 is the greatest headwind. Additionally to the increased cost level due to the pandemic, this includes the impact from accumulated excess mortality in North America and EMEA and the resulting consequences on the efficiency of the operations of our facilities, including downstream assets. There is a limited ability to flex the workforce in EMEA. And in general, this also limits the ability to absorb wage and fixed cost inflation. The lower G&A spend relating to travel, meetings and self-insured health plans is likely to partially reverse in 2021.
Turning to Slide 29. As Rice announced earlier, we plan to launch FME25 to transform our operating model to position our Company for the next 25 years, while we execute on our mid-term strategy launched at our Capital Markets Day in October 2020.
In order to support our 2025 targets to further strengthen profitability and to compensate for the COVID-19 effect, we plan to invest up to EUR500 million by 2025 in order to sustainably reduce our cost base and minimally improve operating income by the same amount. What we mean by this, for example, is if we invest EUR400 million, we would expect to improve our operating income by at least EUR400 million.
FME25 is intended to look at all facets of our global operating model with the intent to simplify, streamline and to apply what we have learned from the COVID pandemic and the resulting new normal. We also see this as an opportunity to further accelerate our digitalization plan. We believe FM25[Phonetic] will be supportive of our mid-term targets, which I will touch on the next slide, Slide 30.
At the time of setting our 2025 targets in October 2020, the COVID impact on our business was roughly net neutral due to various measures and government relief. As it was unclear how the pandemic would evolve, we had excluded impacts from COVID-19 on our 2025 targets. Unfortunately, the development of the pandemic proved this cautious approach to be raised. We have to recognize how significantly the impact of COVID-19 on the achievement of our 2025 targets has increased since then. Of course, we can only anticipate the impacts from the pandemic on these targets based on what we know today, and earlier I outlined our assumptions with the explanation of our 2021 targets.
We do stand by our 2025 targets. In order to achieve those despite the anticipated COVID-19 impact, we will introduce FME25 as a countermeasure in the medium term, but also as a margin driver in the long term.
To be very concrete, in respect to our 2025 targets, we assume that FME25 compensates for the anticipated impacts from COVID-19. Of course, this will change the phasing of our target achievement from equally distributed over the five years to be more back-end loaded by the nature of the transformational change of our global operating model, which we are approaching a positive net income from FME25 is not expected early on. Therefore, we continue to expect revenue growth in the mid-single-digit percentage range and net income growth of high-single digits through 2025 with a changed phasing.
With that, I close my prepared remarks and turn it back to Dominik for, I'm sure, a lively Q&A.
Dominik Heger -- Executive Vice President, Head of Investor Relations, Strategic Development & Communications
Thank you, Helen, Frank and Rice for the presentation. I'm happy to turn it over straight to Q&A. Emma, could you please open the lines.
Questions and Answers:
Operator
Yes. Thank you. Ladies and gentlemen, at this time we will begin the question-and-answer session. [Operator Instructions] First question comes from the line of Veronika Dubajova with Goldman Sachs. Please go ahead.
Veronika Dubajova -- Goldman Sachs -- Analyst
Thank you, guys, and good morning, Helen, Rice. Good afternoon, Dominik. Lots of questions, I'm going to try to stick two, but there might be a third that sneaks in. I apologize. The first one, I want to start with sort of the FME25 program and that up to EUR500 million of investment. Just kind of curious, FME has been restructuring for a long time. This is a pretty significant number. So I'd love to understand your degree of confidence in that EUR500 million or up to EUR500 million of cost savings where precisely those might be coming from if you can give us some examples?
And I guess there is that up EUR500 million, so maybe at this point in time, what do you see as the most likely investment amount? Obviously, I'd appreciate this will change, but if you can share some of that, that would be very helpful.
And then my second question is on excess mortality. And we've spent a lot of time talking about it in the context of your existing patient population. There is, of course, excess mortality also in the broader CKD patient population. And I'm curious how you're thinking that impact that might have in the growth rate in your business as we transition into 2022 and beyond and if you've done some quantification around that? That would be helpful. Thanks.
Rice Powell -- Chief Executive Officer and Chairman
Thank you, Veronika. I think Helen and I will tag team number one. And then, Frank will talk about mortality, both ESKD and CKD. So yes, we have been on cost optimization programs several times in my tenure. And I would say what's different today or going forward with FME25. Those programs were already very -- always very targeted. They were not large amounts of money. If you go back to the old GEP days, we were looking at purchasing synergy, we were looking at shared services and things of that nature that were very targeted. When we had the EUR100 million cost optimization in '19, it was very focused on clinics and FKC, the clinic business if you will, and some of the complementary assets in North America.
Where we look at this up to EUR500 million opportunity is really from an enterprisewide view of the world. We've grown tremendously. We, as you know, operate in 150 countries' product, 50 services, and we built and we are managing people in all of those areas. And I think we are, as a result of COVID, asking ourselves, let's look globally, regionally and locally what does it take to run our business effectively and efficiently having come off a year where we didn't travel hardly at all, we closed the books remotely, if you will, and we've had the opportunity to see these new normals of the way we can do business.
So from my perspective, the difference is this is soup to nuts and it's not a targeted entree, if you will, if we're going to stick with the real analogy. But Helen, let me -- let you get your oar in the water here as well.
Helen Giza -- Chief Financial Officer
Yeah. I think, I would just echo that this is different. This is a global review of our operating model. As we said, looking at where and how we do the work, I think also looking to see where we can leverage digitalization. As we think about this program, Veronika, we are thinking kind of a little bit longer in time, so not just the one or two-year program, I think, because of the holistic nature of this. But the investment phasing and the savings phasing, we have work to do and we would look to come back with more detail as the year goes on.
I think it wouldn't be unreasonable to expect that we could start to see net savings by 2023 and accumulating past then, but we obviously will come back with more granularity on the specific areas. And obviously, there's kind of the usual suspects, I guess, I would say, in terms of as you think about an operating model and locations and things like that, but more to come as we go through the course of the year.
Franklin W. Maddux -- Global Chief Medical Officer
Veronika, this is Frank. Thanks for your question about the mortality in CKD. So there are a number of things at play. We know that the CKD population, in general, is expanding with what Rice mentioned around diabetes, hypertension and other things. But we also know that the pandemic has had a distinct effect as it has in the general population on patients with CKD. In the midst of that, what we have seen are during the surges referral patterns change and also patterns in which patients are getting their routine and usual care that they would get. So it's been very difficult to quantify what these numbers are, but we know that there is an impact in this part of the population that we anticipate will recover as the pandemic begins to recede.
And so we have found as the year progressed and people became more comfortable with treating the pandemic or treating patients in the pandemic, we saw more of our referral patterns recover and nephrologists seeing patients, both virtually and at times of need. And so, I think that this will begin to normalize as the pandemic falls back. But the actual number of CKD patients that are lost strictly to excess mortality, I would look toward the general population rates and create an analogy from that. There is no hard number yet published on this particular area.
Veronika Dubajova -- Goldman Sachs -- Analyst
That's very helpful. And if I can stick in a very quick follow-up on the kind of COVID impact and the cost savings, Helen, any thoughts you have right now on the durability of some of the kind of PPE nursing wage costs? Is that something that you anticipate will continue beyond 2021?
Helen Giza -- Chief Financial Officer
We hope not. We're definitely thinking that our PPE cost will be on a similar level in '21 to what they were in 2020. As far as the additional labor cost for isolation clinics and so on, that had also been a significant -- we expect a significant reduction in '21 to 2020, can't get my years right, excuse me, because of the different nature and the pulsing of the outbreak.
What we're, obviously, trying to do on PPE, in particular, we are using more and we are having to pay significantly accelerate -- inflated pricing. We would hope as we kind of turn the corner here in the back half of 2021 that we will be able to use less PPE and prices will return to somewhat normal. So we're not expecting that these additional PPE costs would continue into 2022 or if they do, it won't be as significant as the level as 2021.
Veronika Dubajova -- Goldman Sachs -- Analyst
That's great. Thanks, guys. I'll jump back into the queue.
Rice Powell -- Chief Executive Officer and Chairman
Thank you.
Operator
Your next question comes from the line of Patrick Wood with Bank of America. Please go ahead.
Patrick Wood -- Bank of America -- Analyst
Perfect. Thank you very much for taking my two questions. The first one please, could you give us a little bit of color may be more on the Medicare Advantage sign-ups and how you've seen that going? And equally on that vein, the contribution in '21 assumed from value-based care from capitas agreements, it seems larger than I would have expected. Just a commentary around that. So that's the first question.
And then the second question, if you could maybe give us a little bit of a sense from the impact that you've had or expect to have next year for missed treatments, right, because I'm guessing there's also a lot of patients who are electing to skip a treatment, maybe do two a week or some alternative rather than turning up or alternatively are now getting treated in the acute setting rather than in a clinic for different reasons. How -- because it's not quite the same effect as mortality, how should we be thinking about that impact? And does that roll back in, in '21 through the year as we go through? Thanks.
Rice Powell -- Chief Executive Officer and Chairman
Sure. You want to take one? I'll take two.
Helen Giza -- Chief Financial Officer
Sure. Happy to. Hi, Patrick. I'll take the Medicare Advantage. So as we had been sharing with you guys at the end of last year, we were seeing our Medicare Advantage business at the high-teens at the end of 2020. We were encouraged with the enrollment. It went very smoothly. And we -- the outcome was in line with our expectations, and we have seen the uptake in the mid-20s currently.
Obviously, as the course of the year goes on, we're able to -- there's more opportunities for enrollment and we remain encouraged on this book of business and still believe that it could be in the mid-30s in line with the general Medicare Advantage population. So yeah, our expectations were met and we're very, very happy with how that came in. Rice, you want to take value-based care?
Rice Powell -- Chief Executive Officer and Chairman
Yeah. So Patrick, when we look at value-based care, a couple of things that will probably point in the right direction. We are operating today in the U.S. with roughly 25% of our patients in value-based care arrangements. We've got around 43,000 that are in the ESCO program that will move into the new models as we get through Q1. And then in our Medicare Advantage value-based care operations, we're looking at around 10,000 patients. So this is significant for us. It's a quarter of our population. And I think it's the strength of what we've been able to deliver in terms of better outcomes and good savings that are helping us drive this. We are quite active in this. We've always said this train has left the station for us. It is going to be the way we continue to see, I think, large growth opportunities as more people come into value-based care.
And then, your second question on missed treatments. We don't see an increase there. We see missed treatments at kind of a level that we've always seen them. No doubt when we got into the first wave back in 2020 and there weren't any opportunities for people initially to get into treatment, they were worried about it. We found a way to make sure we could work with people. If you remember, we got a number of waivers. We could help people get transportation to get into their treatment.
So I think from a missed treatment standpoint of people alive and well, but deciding I'm not going in, I don't think we're expecting to see that become a thing, if you will, particularly in the U.S. And keep in mind and in some of the emerging markets, two treatments per week is the norm. So in our very developed markets, we're still looking at the three times per week. So we don't really see that as something that would be a headwind for us in the course of this year, '21.
Patrick Wood -- Bank of America -- Analyst
Super. Very clear. Thanks guys.
Rice Powell -- Chief Executive Officer and Chairman
You bet.
Operator
The next question comes from the line of Lisa Clive with Bernstein. Please go ahead.
Lisa Bedell Clive -- AB Bernstein -- Analyst
Hi, there. First question, DaVita had indicated that they saw increase in mortality as about 7,000 patients in their U.S. business and this is about a $200 million headwind, so around $20,000 per patient. Given these, said you had 10,000 patients and your U.S. business is very similar to theirs, is it safe to assume that your split, maybe something like 7,000 in the U.S. and 3,000 in Europe? And on the cost front, you did mention on the call, I think you did, the labor costs are more fixed in that region. So is it safe to assume that the EMEA headwind per patient is greater than the numbers that DaVita had implied?
And then second of all, just looking at your international business, obviously, kind of ignoring last year because of the pandemic, but the services business does seem to just be getting less profitable over time. Can you tell us what is built into your normal contracts around inflation adjustors? You often do mention that you sort of have labor costs running up. I'm just trying to understand if this is just a sort of perpetual squeeze that you may see or whether you do end up getting compensated for that eventually.
Rice Powell -- Chief Executive Officer and Chairman
Okay, Lisa. Frank, why don't you jump in on the mortality and what she's asking about there relative to the split?
Franklin W. Maddux -- Global Chief Medical Officer
Yeah. So Lisa, this is Frank. So our split overall was about 10,000 excess deaths across the globe. And when we look at the U.S., our U.S. component of that was somewhat less than what was reported in the other earnings call, and it is 6,000 patient range.
What we did see was a distinct difference in the early waves where there were far fewer excess deaths in EMEA, but this very last wave was quite substantial. And in the EMEA region, we have clearly seen this sort of winter wave being the more substantive COVID exposure that was seen in those particular areas. So our ultimate aggregate result is in aggregate from all four of the regions, and that is -- that's kind of how the split works.
Rice Powell -- Chief Executive Officer and Chairman
So Lisa, on headwinds for EMEA. Yes, I mean if you look at labor costs and the ability to manage that labor cost under a situation like this, it's a little bit tougher in EMEA for them to do that. It's not as -- it's a lot more complicated in the way we operate in the U.S., if you will. So I think there are some things there that we don't have as many degrees of freedom, if you will, depending on the market that you're in.
And then on the services margin internationally, I would say, and particularly in Europe, remember that when you go back and you think about percent product business versus percent service business, as that service component grows, you get margin pressure because of the labor component of that. And so that is just kind of -- as you all know, that's just kind of a progression that we go through. So we have to find other ways within the service sector to be able to try to combat that.
I would also say one of the things that we have observed latter part of 2020 is that there are some markets, Hungary, Poland, the Czech Republic, that as they have kind of taken a more nationalistic view politically, we have been sort of dictated to in terms of what pay is going to be, what the rates are going to be for nursing pay, etc. They're trying to help uplift their economy and hang on to their nursing staff and not have them leave that country go someplace out. So all of those things have worked against this to some degree and have created a little bit less flexibility than perhaps we're used to in other markets.
Lisa Bedell Clive -- AB Bernstein -- Analyst
Okay. Can you just -- do you have inflation adjustors built into this contract? There it seems like some of these are very sort of country-specific and it's sort of out of control?
Rice Powell -- Chief Executive Officer and Chairman
Yeah. No, we don't really have that. It's not something that we are able to do, which is put inflation adjustors in our negotiations with countries relative to what they are viewing healthcare pay to be, if you will. That's not something that we really have an opportunity to do.
Lisa Bedell Clive -- AB Bernstein -- Analyst
Okay, sorry. And then last question, on MA, you said you had about 10,000 patients capitated or rather in value-based care. I was under the impression that a standard contract alone would be bigger than that given how big they are in MA. So are those numbers from 2020? And will the expanded Humana contract significantly change that number?
Rice Powell -- Chief Executive Officer and Chairman
Yeah. So you're smart to peg it to a date. So that's kind of what I would say where we're exiting and stepping off into the new year. So give us time as we work quarter-to-quarter and ask me again and I'll give you an update. But obviously, the Humana contract is just getting kicked off, so we've got some things that will have to happen there as well.
Lisa Bedell Clive -- AB Bernstein -- Analyst
Perfect, thanks.
Rice Powell -- Chief Executive Officer and Chairman
Sure.
Operator
The next question comes from the line of Tom Jones with Berenberg. Please go ahead.
Tom Jones -- Berenberg Bank -- Analyst
Good afternoon. Thanks for taking my two questions. Apologies to Rice and Helen, but they are both for Frank. Frank, thank you very much for the data on -- that you shared on this sort of uniform mortality you're seeing from an age perspective. But I wondered if you can make any comments around mortality if you split your patient base into kind of comorbidity view? And also highlight to that, maybe this question more for Rice and Helen, is there -- are you seeing any significant differences in mortality when you cut the patients by payer type?
The second question I had was just on vaccination in your patients. Could you give us an update on where you are vaccination-wise and also whether you have any at least early stage data on the efficacy of vaccinations among your patients? We are starting to see some early data coming out in real world use for broad populations for the efficacy of vaccines when it comes to reduced mortality and hospitalization, but I was just wondering if there was any early data you could share on this type of vaccines appear to be having on mortality and hospitalization, specifically among dialysis patients?
Franklin W. Maddux -- Global Chief Medical Officer
Great. Thanks, Tom. So let me with start the first one, looking more broadly at age and comorbidities. When we've looked at the way that we capture comorbidities around pulmonary disease, cardiac disease and other things, what we see over time is the same stability over the years that we have looked at where we look back the last three years. So we have very, very little change in what the end-of-year rate year-over-year is of this -- of the comorbidity profile of the patients that we have.
We have not looked specifically in our medical office at payer type, so I can't answer that question directly. But what I would tell you is we have analyzed deeply that in individual patients, chances of infection and the prediction of whether they are more or less likely to get infected is most consistent with the ZIP code that they live in. And so it is very geographically oriented to the background rate of community infection that's seen in those ZIP codes. So if you have a person living in a very densely populated area and small location, they are at a higher risk than somebody who is living in a very rural community as an example or not around a lot of other people. And as that might track toward payer type, you might be able to infer something there, but we don't have that, we've not looked at that.
From the vaccination status, I would tell you that around the world, the vaccination progress is highly variable and except in three locations that we have, has been relatively insufficient to what the herd immunity needs are. What we have seen is some remarkable vaccination projects that have been completed in Portugal, in Israel and in Puerto Rico. And each of these took a different path toward vaccinating the population in our patients. There is active work being done to begin to analyze the ultimate impact on these patients. We are in active studies right now to look at the immunologic response to vaccination in dialysis patients, which if you look at Hepatitis B vaccination and influenza vaccination, there's an attenuated immune response in our target population of patients. And so we will be looking at that with both the mRNA viruses and the adenovirus vector viruses that are out there.
The second thing we could see is when we look at first doses in our two largest regions, EMEA and North America, we see sort of mid- to high-teen range of first doses having been given as of this week and we have a small number of single-digit percentage of patients that have had doses -- second doses given. And then finally, we are seeing -- we are just beginning to unpack some of the vaccine hesitancy that we've seen, and we see a slightly lower vaccine hesitancy rate in our patient population than our staff population. That's kind of what we -- where we are on the current status of vaccinations, Tom.
Rice Powell -- Chief Executive Officer and Chairman
Tom, the only thing I would add is that each of the regions where possible is trying to engage with the local governments to allow us to be a [Technical Issues] nation because we do the flu vaccines every year, we do the hep B, etc. And specifically in the U.S., we started back in mid-December at a very senior level here in North America and with our government affairs, people talking to CDC and the government, about allowing us to be a licensed vaccinator, if you will, giving us the impetus to be able to do this.
We've also had some state-to-state discussions. It is slow. It's somewhat bureaucratic, but I think at the end of the day, we'll keep pestering people until they allow us to do this because we just think it makes the absolute most sense to not take somebody out of a dialysis clinic and ship them over to a gymnasium across town to get them vaccinated. And I just think we have to keep working with it. The change of administration creates some uncertainty as well. But all of those things, we're just going to deal with them and keep pushing ahead because we think we can play a vital role in this and do it in a way that's better for patients and staff.
Tom Jones -- Berenberg Bank -- Analyst
Why do you think there has been such resistance because I assume availability of vaccines is the only thing that's limiting your ability -- really limiting your ability to vaccinate patients? And if you're wanting to get a benefit, if you look across your patient base with the generally older, they are mostly diabetic, a lot of them are obese, they've all got high co-morbidities and lot of them are African-American. And you've got doctors and nurses, they are ready to do the injections and deal with any adverse events that may occur. So I'm amazed that any government around the world is not just giving you the vaccine straight away and letting you get on with it.
Franklin W. Maddux -- Global Chief Medical Officer
Tom, this is Frank. We would agree with you on that statement. And I would say in the areas where we've seen quite effective vaccination programs. In Israel, the healthcare system brought us directly to patients and our patients as opposed to patients having to go to it. In Portugal, the distribution was directly to our clinics. And in Puerto Rico, it was a National Guard effort. It was sort of a public local use of sort of the National Guard to try to make sure there was broad distribution to the population.
So our -- the work that Bill Valle and the team has done and Cam Lynch in D.C. to try to get vaccine delivered directly to our clinics, both for our clinics and the rest of the renal community, has been one of the central efforts that's been going on. And we're still hopeful that we will get there. But it has been plagued by a lot of logistical and I think political changes.
Tom Jones -- Berenberg Bank -- Analyst
Okay, that's very clear. Thanks.
Rice Powell -- Chief Executive Officer and Chairman
Sure. Thanks, Tom.
Operator
Next question comes from the line of Oliver Metzger with Commerzbank. Please go ahead.
Oliver Metzger -- Commerzbank -- Analyst
Hi. Thanks a lot for taking my questions. First one is on -- also in excess mortality. So you've specified about 10,000 patients who passed away incrementally. Also you provided some data points for mortality among the quarters. Could you give us an indication about the distribution in the fourth quarter? So, with 3,007 [Phonetic] excess deaths and potentially starting from the mid of November or potentially from beginning of December until the end of the year, so for a period when infection rates have started to peak.
The second question is also on the similar directions. So the patients who unfortunately passed away appear to be more severe sick dialysis patients. Frank, you made already some comments on this. I believe you collect a lot of data and do a lot of analytics. Could you share with us your view on average life expectancy of the patients who passed away? My question targets toward the timeframe when you would reach normalized patients of [Indecipherable] pre-corona patient structure again.
Franklin W. Maddux -- Global Chief Medical Officer
Oliver, thanks. Do you want me to take that one?
Rice Powell -- Chief Executive Officer and Chairman
Yeah. No, please go ahead.
Franklin W. Maddux -- Global Chief Medical Officer
Yeah. So on the phasing of sort of what we're seeing, the graph that I showed you in the fourth quarter is recognizing that there are seasonal trends that show increased deaths in a typical normal year due to influenza-like illnesses that occur. So when we looked at the excess death rate, you have to look at when we saw the peak exposure in the two main reasons -- regions. So EMEA had the largest peak in December, and so we began to see impact on the mortality rate from EMEA in these final weeks of the year that began to accumulate toward that 3,000 or so that you saw in the fourth quarter.
In the U.S., that peak, if you look at it on a week-by-week basis, did not occur until around the second week of January. And at that time, we are now capturing the data from that particular peak. And so although there were excess deaths obviously from the ongoing evolution of this third wave in the U.S. and this effectively second wave in EMEA, I think the proportion of those patients that were EMEA patients was probably higher in the fourth quarter than it had been in the prior quarters. And the impact that we are seeing from the third wave in the U.S. is part of the early 2021 impact that we expect to see.
Rice Powell -- Chief Executive Officer and Chairman
I think, Oliver, also, it's Rice, I think one of the things that you kind of have to factor in as you work your way through this and you think about it, none of these mortality situations, none of these patients passed in our clinic. They are passing away in the ICU, in the hospital, perhaps in a nursing home. The nephrologist does not -- I hate to say it this way, but they don't do the death certificate. It's coming from a different physician. And we many times are not finding out about that passage for four, five weeks or something like that. So we're not even getting awareness of the passing until it's probably a month later.
Franklin W. Maddux -- Global Chief Medical Officer
The other thing which we found is that in the initial stages of the pandemic back in March of 2020 and April 2020, we saw deaths occurring very concurrent with the identification of disease. As health systems begin to understand how to begin to organize and treat patients with the disease, we saw a wider array of patients with varying degrees of illness with COVID and we saw that patients were living longer under more intensive care -- in intensive care units and hospital systems and so forth. So it took longer for those deaths to occur than what we saw originally, and that was true in all three of the waves that we saw.
On your second question with regard to the degree of illness that people have, what we've been looking at primarily is trying to recognize that the pandemic is a pandemic that broadly affects the vulnerable population of kidney patients. It is not a single age group. It is not a single profiled comorbidity. It has occurred across all of these patients to a degree, some to larger or lesser degrees. But when we look at what the impact and what our population looks like today, the data doesn't tell us or doesn't show that, in fact, we've had significant changes to date in the profile of the patients we treat. So whether it's comorbidities, whether it's age or other things, we have seen that the impact of the pandemic has actually spread through a pretty wide swath of the population of patients that we do treat.
Now, this may change as we get further information from the third wave, but to date, that's what the data shows us. And we've been trying to be extremely objective about how we look at this. The other thing that has occurred is when we see the excess mortality surges that occur either just after a surge in cases, in between those surges, there is a return toward normal, but we have yet to see any return all the way to normal. Between the first and second surges, there was a return back toward normal, but it didn't make it all the way back to our baseline. And the same occurred between the second and third waves.
So we still -- we'll see what that baseline normalcy looks like as we actually exit the pandemic. I hope that helps.
Oliver Metzger -- Commerzbank -- Analyst
Yeah, yes, it helps. But could you make a comment just on this topic of life expectancy? So how does life expectancy for patients who passed away compares to your average life expectancy of your normal dialysis population?
Franklin W. Maddux -- Global Chief Medical Officer
So our normal dialysis population, the life expectancy of somebody that's symptomatic with COVID is quite a bit shorter, obviously, and otherwise, we wouldn't have seen these excess deaths that are from COVID. And so I would say the degree to which that occurs is a little bit difficult to quantify, but I would tell you that it's substantially different than the baseline.
The baseline has been many, many years. For a person that's COVID positive, we are now finding that there are patients that are asymptomatic dialysis patients with COVID, and then there are obviously the many symptomatic patients. So I think it's a difficult question to actually answer directly. But simply to say that if you have COVID, you develop severe symptoms, your risk of death is much, much higher than it might normally be, and that may be even an order of magnitude higher.
Oliver Metzger -- Commerzbank -- Analyst
Okay. Thank you. The next question comes from the line of Michael Jungling with Morgan Stanley. Please go ahead.
Michael Jungling -- Morgan Stanley -- Analyst
Thank you, and good afternoon and good morning all. And I have two questions. Firstly, on mortality. In the presentation or so, you mentioned 10,000 excess deaths. Where do you think you'll be by the end of this year? Are we talking here about sadly 20,000 people or is it slightly more or slightly less? And the context of mortality, do you have a sense of what percentage of your ESRD patients have already had COVID-19? I suspect you do some antibody testing.
And then finally, question two is on the CARES 2 program for a lack of a better word. How would you assess the lobbying of getting more government aid or support in Washington in 2021? Is there some sort of catalyst or event that you're focusing on that would make such a decision perhaps reality? Thank you.
Franklin W. Maddux -- Global Chief Medical Officer
So Michael, thanks. This is Frank. I'll start with the first two. And predicting mortality is incredibly difficult in this disease. And I think that some might have predicted but some might not have predicted that there would be a third wave. And I think not knowing the impact that these genetic variants, whether it's the U.K. variant, South African variant or a new variant that will occur, I think we can predict that we will be living in a world with the pandemic.
But the impact of additional surges is going to be based on a lot of things that we either don't control or don't have visibility on, such as vaccination rates and getting to the point of herd immunity quickly. Genetic variation and whether the vaccines will be sufficiently stimulus for an immune response against those particular variants, whether we will have economies opening up faster with reduction in non-pharmaceutical interventions like social distancing and masking that will impact spots that flare up in surges. All of those are going to impact what our ultimate rate is. And the degree of discipline that we see country by country is, frankly, quite different.
And so all of those things are going to be the reason why I use the word dynamic in my prepared comments because I don't think we know the answer to that question. I don't think there is really a good answer. We know that the third wave that there are excess deaths that extend into 2021. And as we stated, we anticipate that they will extend through a proportion of this year.
Now the incidence rate, I can tell you that if we look at our global case rate of COVID, we've been able to -- through testing with PCR testing, recognize that 60,000 patients have had COVID that we have cared for around the world. And that was a number from a week or so ago. It was right at 60,000. And so we know that, that's kind of the incidence rate that we're seeing on there. And then I'll turn it over to either Helen or Rice to answer.
Helen Giza -- Chief Financial Officer
Probably, Rice will take.
Rice Powell -- Chief Executive Officer and Chairman
Yeah. So Michael, here's where we are. Had lots and lots of discussions with the incoming folks and the Biden Administration and both sides of the aisle as well Publicans and Democrats. It would appear at this point that the $1.9 trillion bill that has been put together that has not been acted on, we're hearing that they want to act on that middle of March. And what we're hearing there is, at this point in time, there is no relief included in that package for providers. So, we are engaged in having discussions and trying to understand that. But that is a very clear answer that I have personally gotten.
Secondly, in the provider relief fund that was appropriated under the Trump administration, there's around $30 billion money available. And the way you access those funds during the Trump administration, as we have been told is going to be different under the Biden administration. We are asking and waiting to understand and get some guidance on what are the rules of the road going to be per se, but we've not gotten any feedback on that as of yet.
So again, we believe our assumption of no relief is prudent at this point, and we have to see what comes out of the mid-March activity and the larger bill that at this point, we're told there is no provider relief and then still waiting to get some sense and idea of what the process will be for the provider relief funding that was explicitly put together for providers, be that hospitals or dialysis providers. We're waiting to see what's going to happen there.
Michael Jungling -- Morgan Stanley -- Analyst
Okay. Great. And briefly follow up on those patients who have been diagnosed with COVID and have survived, are they more difficult to treat as a result of the disease? Meaning, as they get better, are they even if I can use the word iller or are they even unhealthier that the cost also of treating those recovered patients is higher, or is the mortality or life expectancy lower once they've survived COVID in the first place? Do you have some sort of data, which would suggest some sort of trend? Thank you. Sorry for the follow-up. Thank you.
Franklin W. Maddux -- Global Chief Medical Officer
Sure. So there's no evidence that they're any more difficult to treat. They obviously, after COVID goes through a period of recovery. And as you know, there are sequelae to COVID that require a fair amount of time to get over. But the treatment for their renal replacement therapy is no different and the types of work that our physicians and nurses are doing is essentially unchanged. We do try to protect these patients from getting reinfected. And so, they are observed very, very closely during these times, but effectively no distinct treatment.
Now, those with COVID are being afforded the available treatments that are -- we've made available antibody treatments. We've made available other treatments that give them the opportunity to try to recover. But it's a -- but it effectively from the dialysis standpoint is not substantially different.
Michael Jungling -- Morgan Stanley -- Analyst
Thank you.
Franklin W. Maddux -- Global Chief Medical Officer
Thank you.
Operator
The next question comes from the line of David Adlington with JPMorgan. Please go ahead.
David Adlington -- JPMorgan -- Analyst
Thanks, guys. Also for Frank please. So just on the patient outcome slide, I was intrigued to see that your patient hospital days have actually come down a little bit year-on-year, which seems odd given the excess deaths and I expect some of these patients to end up in hospital before. And so, it would be good to get your thoughts on that first.
And then just to sort of circle back on that sort of 10,000 deaths out of 60,000 patients you had. It's obviously -- that looks like one in six death rate. Is that fair? And I think that does sort of put you in line with that the order of magnitude higher in a general population in terms of mortality rates?
Franklin W. Maddux -- Global Chief Medical Officer
Great. Thanks. So the hospital day is coming down in a couple of regions. I think is actually -- it's counterintuitive, but it makes sense when you realize that as surges occurred in communities, hospitals were overwhelmed with caring for COVID. And that caring for COVID in the general population reduced a lot of routine care that was occurring in hospitals. And patients didn't want to go to ERs, where there were a lot of COVID patients and they didn't want to go be placed into hospitals.
And at the same time, the routine care was disrupted especially earlier in the course of the pandemic. So, we saw hospitalization rates typically fall in those areas, where there were surges and there was overwhelming pressure on the healthcare system from COVID. And so, that counterintuitively is one of the things.
Now with the 10,000 deaths from the 60,000 cases, remember the 60,000 cases are the cases that we have diagnosed with positive PCR testing. Not all patients are diagnosed and not all of the excess deaths are in people that are known to be COVID positive. And so, there is a -- probably -- and this is seen in the general population as well, the actual rate both on the mortality side from COVID and on the exposure side of being able to identify patients with COVID is probably quite a bit higher than what's actually documented. So I think the 1/6th death rate is probably not accurate as an assessment of that because of those reasons.
David Adlington -- JPMorgan -- Analyst
Great. Thank you.
Operator
Next question comes from the line of James Vane-Tempest with Jefferies. Please go ahead.
James Vane-Tempest -- Jefferies -- Analyst
Hi, good afternoon. Thanks for taking my questions. It's James Vane-Tempest from Jefferies. Rice, can you clarify the up to EUR500 million investments and timing for those to be cost savings? I mean, I understand these are in the preliminary stages. So, for example, you spend EUR50 million this year, I appreciate it depends on what these are but I'm just curious of the timing how you'd expect to be benefits over time?
And then second question if roxadustat gets approval and stay on the funding, I'm just wondering how you have this opportunity for Fresenius in the U.S.? And is there any contribution from that included in your guidance? Thank you.
Rice Powell -- Chief Executive Officer and Chairman
Go ahead.
Helen Giza -- Chief Financial Officer
Yeah. Hi, James I'm happy to take the FME25 question. So, yes, you're right. The -- depending on what it is will depend on the wage a savings capture. I think if you look at real estate or facilities versus people, you get a quicker payback or things can take longer. I would say on average, we would expect payback within three years. And then that payback is going to be phased over the next few years as we tackle these different elements of our operating model. And that is, obviously, the more detailed work that we have ahead of us, and I think we'll be able to give more of an update on that as I mentioned when we come back at Q1.
And obviously different parts of the world have different restrictions on how quickly you can do something, but would be -- the sizing of it I think that was the other part of your question. We're not just looking at this for how do we counter the impact of COVID. But as part of our Capital Markets Day target, we always had margin expansion in there. So we feel that the EUR500 million is the right size to get through this mid-term target and set us up for sustainable profitability beyond.
Rice Powell -- Chief Executive Officer and Chairman
James on roxadustat, no, at this point we've got no assumption that that will be approved and it will be running through our P&L in the 2021 plan at this point.
James Vane-Tempest -- Jefferies -- Analyst
That's great. Thank you.
Rice Powell -- Chief Executive Officer and Chairman
Sure.
Operator
Next question comes from the line of Silke Stegemann with Deutsche Bank. Please go ahead.
Silke Stegemann -- Deutsche Bank -- Analyst
Thank you. I would have two questions as well please. Firstly on Medicare Advantage, could you share when you think you can reach the mid-30s threshold that you mentioned earlier in your prepared remarks? And then secondly, could you provide a bit of an outlook for your dialysis products business for the year? Do you expect some weakness here as part of this excess mortality situation, or do you think the products business can still post solid growth again in 2021?
Rice Powell -- Chief Executive Officer and Chairman
All right. Helen, do you want to take Medicare Advantage?
Helen Giza -- Chief Financial Officer
Yes. Hi, Silke, so what we've always said is we feel we can get to that mid-30s. The trajectory and the enrollment and the time line to get there is somewhat out of our control. We feel -- we did this enrollment through a third-party broker and it was incredibly successful. The North America team did a terrific job with this. Obviously, it's about patient education discussion with the physician on the different benefits that the plan offers. I think we ask ourselves why in time wouldn't the patient take a Medicare Advantage plan, and obviously it comes down to consumer choice. So I think within the next couple of years we could see that mid-30s, but I think we'll see what happens in the next round of open enrollment. I think by the end of 2021 we'll be more informed on how that uptake looks going into 2022.
Rice Powell -- Chief Executive Officer and Chairman
Silke, hi, it's Rice. Products growth, I think one of our advantages is having a complete full product line for all dialysis products is advantageous for us. We still are believing and planning on growth in products this year. Given the fact that we can see a need in the critical care space particularly as we've said we believe COVID's going to be here at least through H1 that will create opportunity for us from an acute care standpoint.
As you well know the disposables become the blade if you will. So they are going to continue to be sold for in-center patients as well. We do anticipate maybe some softness in our in-center machine business, but we've seen that from time-to-time. But at this point, we are looking at growth for the products business -- we'll have the opportunity to generate that kind of I would say mid-single digit somewhere in that range growth.
Silke Stegemann -- Deutsche Bank -- Analyst
Okay. Thank you.
Rice Powell -- Chief Executive Officer and Chairman
Sure.
Operator
Next question comes from the line of Christoph Gretler with Credit Suisse. Please go ahead.
Christoph Gretler -- Credit Suisse -- Analyst
Thank you, operator. Hi, Rice. Hello, Frank. Still two questions left. The first is on your guidance, net income guidance. I mean, in a historic context at least it's a pretty wide range high-teens to mid-20s now it's almost more than EUR100 million net income essentially. Now if I look at kind of your assumptions and kind of the key element that could drive. It -- I mean some of them are known. I mean, you knew how much money you got from government last year kind of the pandemic-related costs. We also now have a pretty good kind of sense about the level et cetera. So I mean, could you maybe expand a bit on what is required to get to the low-end what required to get to the high-end and what is probably the most kind of critical and most variable factor maybe behind this relatively wide guidance range?
Helen Giza -- Chief Financial Officer
Yeah. Hi, Chris. This is Helen. I'll take that. So yes, you're right. It is a range that is somewhat deliberate. I think the -- obviously as you can see from our headwinds and tailwinds, we have a lot of moving parts in 2021. I'm very confident on our operational excellence that we will deliver what we're good at and the fundamentals of our business is strong and the operating model is strong. For me, I think the biggest variable quite honestly is the mortality. And what we really see is the continued trajectory going into half one coming off the back of some pretty big numbers in December and January. So obviously with a lot of questions for Frank today on mortality and vaccination, but I think those two things are going to be the game-changer for us in 2021 and when we start to tip over on that curve. So I think the rest we know how to manage. But that one in particular is somewhat harder to call. So I would say that's the biggest variable.
Christoph Gretler -- Credit Suisse -- Analyst
Okay. So then at least there is hope that maybe if we progress in the year that you're going to tighten it. And then the second question is just on care coordination. I noticed that after minorities, it basically turned to loss-making. And I guess what you mentioned it can be good for kind of that business as well. So what's kind of the midterm outlook here now kind of are we now having restructuring candidate, or basically, how would you kind of seen and all the way back to -- I think in the past you saw kind of double-digit margin levels as achievable? Is this still kind of something that is realistic?
Rice Powell -- Chief Executive Officer and Chairman
Yeah. So Helen, and I, we'll double team this Chris. It's a great question. So a couple of things just to get you thinking about it. As we continue to make the migration to value-based care, we require these complementary assets. The pharmacy, the vascular access which is not only renal as well as cardiovascular and things of that nature. So I would say you, as we get through this mortality effect that Helen spoke about and we move beyond that, we would expect to see some improvement because we're going to be able to have patients coming in. They're going to need vascular work et cetera et cetera. Value-based care these complementary assets are so important because that's how we manage the clinical interventions. And we keep patients out of the hospital and we drive higher clinical outcomes.
So as we think about relooking at our business and what we're doing, we're not thinking that we would go in and take complementary assets and just kind of drop them out of the picture because then it makes it difficult for us to be able to manage effectively in value-based care and we've learned this obviously over a number of years. Helen, do you want to add?
Helen Giza -- Chief Financial Officer
Yeah. Yeah I perhaps just would add Chris for us as we think about care coordination and as we take care of these patients and we are moving obviously way more into a value-based care environment. We are likely going to fold in the care coordination reporting into our services report and moving forward. We think that makes more sense to have a more holistic view. And maybe the only other thing I would add is kind of maybe the care coordination segment in Asia Pacific also continues to grow. That's been a successful venture for us particularly in Australia and Idea Of Care clinics for example. So we like the segment of care coordination. We feel it does enable us to offer greater wrap around -- surround I call it for our patients, but it's obviously becoming much more part of our services offering as we move forward.
Christoph Gretler -- Credit Suisse -- Analyst
Yeah. Fully understood. Thank you.
Rice Powell -- Chief Executive Officer and Chairman
Thanks, Chris.
Operator
Ladies and gentlemen, unfortunately we have no further questions at this time. I hand back to Dominik for closing comments.
Dominik Heger -- Executive Vice President, Head of Investor Relations, Strategic Development & Communications
Okay. Thank you, Emma. So we have more questions I know, but we did run out of time even the extended time frame. So I apologize for that. We should have planned for even more. With that, I will nevertheless close the call. I can only say and that more than ever stay safe and hope to hear you soon. Take care.
Rice Powell -- Chief Executive Officer and Chairman
Thank you everyone. Be safe be well.
Operator
[Operator Closing Remarks]
Duration: 97 minutes
Call participants:
Dominik Heger -- Executive Vice President, Head of Investor Relations, Strategic Development & Communications
Rice Powell -- Chief Executive Officer and Chairman
Franklin W. Maddux -- Global Chief Medical Officer
Helen Giza -- Chief Financial Officer
Veronika Dubajova -- Goldman Sachs -- Analyst
Patrick Wood -- Bank of America -- Analyst
Lisa Bedell Clive -- AB Bernstein -- Analyst
Tom Jones -- Berenberg Bank -- Analyst
Oliver Metzger -- Commerzbank -- Analyst
Michael Jungling -- Morgan Stanley -- Analyst
David Adlington -- JPMorgan -- Analyst
James Vane-Tempest -- Jefferies -- Analyst
Silke Stegemann -- Deutsche Bank -- Analyst
Christoph Gretler -- Credit Suisse -- Analyst