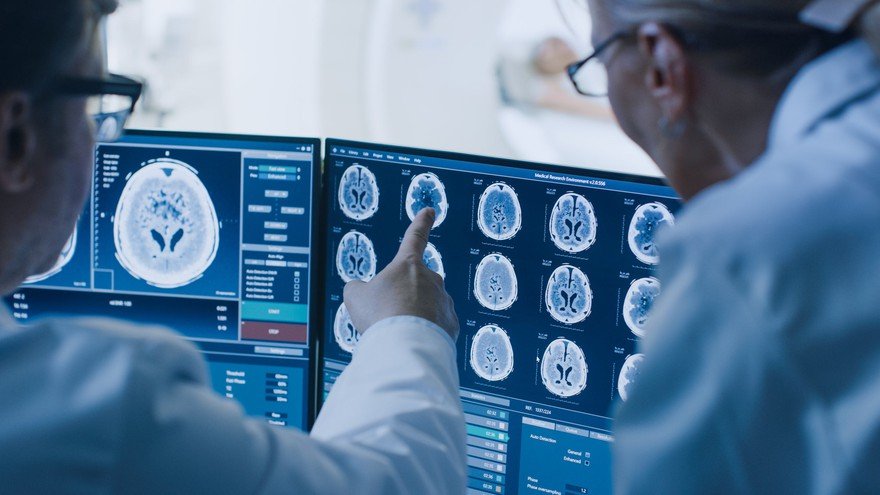
Source: Merck.
There is perhaps no indication more coveted by drug developers right now than cancer care research. Last year, per IMS Health, cancer drug sales hit $100 billion, and by 2018 cancer drug sales could soar another 47% to $147 billion if the high-end of IMS estimates are met.
Cancer immunotherapies are in focus
Although there is no shortage of ways to approach cancer care research -- inhibiting blood vessel growth, stopping the replication process, or seeking out hypoxic tumors are just some examples -- immuno-oncology is getting the most publicity by far.
Cancer immunotherapies are a relatively new approach to cancer treatment. Instead of developing a therapy designed to alter cancer cells, the immunotherapy is designed to heighten the ability of a patient's immune system to locate and destroy cancer cells. Cancer has a way of going undetected by the immune system, so many of these vaccines attempt to remove this immunosuppressant quality and give the patient's immune system a fighting chance.

Source: Bristol-Myers Squibb.
The two best-known cancer immunotherapies are checkpoint inhibitors from Merck (MRK +2.55%) and Bristol-Myers Squibb (BMY +1.73%) known as Keytruda and Opdivo, respectively. Both companies are running dozens of ongoing studies for their respective cancer immunotherapies, with the goal of testing them as both monotherapies and in combination with other experimental and approved cancer care therapies.
The results from clinical studies thus far have been encouraging, with checkpoint inhibitors like Keytruda and Opdivo living up to their hype. Both drugs are already approved to treat advanced cases of melanoma, and they've shown remarkable response rates in select non-small cell lung cancer patients. Keytruda demonstrated a 45% overall response rate in high PD-L1-expressing patients in phase 1 trials, while Opdivo had its label expanded to treat NSCLC in the U.S. in March after delivering a 15% objective response rate in patients who progressed following a platinum-based therapy and at least one systemic regimen.
We're really just seeing the tip of the iceberg when it comes to cancer vaccines.
Price is an issue, and Merck just caved
But a revolutionary product often comes with something else -- a revolutionary price tag. A full year of treatment with Keytruda in the U.S. comes with a wholesale price tag of $150,000, and Opdivo is not far behind with a wholesale annual cost of $143,000. These prices might seem borderline insane, but it fits the profile of a first-in-class new cancer therapy that's highly specialized to a specific type of patient. As personalized medicine continues to evolve, five- and six-digit annual price tags could become the norm.
Of course, not everyone is willing to play ball.

Source: Merck.
Earlier this week we discovered that the National Institute for Health and Care Excellence, affably known as NICE, wasn't going to live up to its moniker. NICE is Britain's watchdog group that helps develop clinical guidelines for new therapies, and it wasn't thrilled with Keytruda's high price point. In fact, it had been rumored that Keytruda's not-so-modest price point could keep it off the reimbursed medicines list in Britain. Ultimately, per a Reuters report, Merck agreed to offer a discount to the state health service, although the magnitude of the discount is being kept confidential according to NICE.
In short, NICE laid out an ultimatum, and Merck caved on its price request (as have a number of other drug companies over the years). Could Bristol-Myers Squibb's Opdivo, or any other number of high-priced cancer therapies, be next?
It's certainly possible in select developed overseas markets. NICE has excluded Roche's Avastin and Pfizer's NSCLC drug targeting the ALK-positive mutation Xalkori because of price. With Keytruda and Opdivo essentially targeting the same pathway, it's always possible that any EU-based regulatory body could decide to play Merck and Bristol-Myers against one another to net the biggest gross-to-net discount imaginable. If you're curious, Opdivo is already approved for NSCLC in Britain with a monthly price tag of $8,800, a $3,100 discount from its monthly price in the United States.
This may not be an issue in the U.S.
Though Merck may have caved in Britain on pricing (even if we don't know by how much), patients in the U.S. are unlikely to see much in the way of price cuts anytime soon.

Source: Flickr user StockMonkeys.com.
There are actually a number of factors that suggest pricing in the U.S. for cancer therapies will continue to remain high. To begin with, drugmakers typically use developed countries (especially the U.S.) to build their profit margins. The high profits realized in the U.S. help to subsidize care given in poorer countries that otherwise could not afford five- or six-digit annual costs.
Also, drug developers have a veritable sea of costs they need covered. They have to cover the costs to develop and market the drug, as well as the cost of recouping some (or all) of the costs of other drugs that didn't make it to pharmacy shelves. And don't forget about litigation costs to protect patents in court.
But the biggest reason U.S. prices for checkpoint inhibitors and other cancer drugs will likely remain high is that insurers and pharmacy-benefit managers (PBMs) in the U.S. have minimal power to control drug pricing. Congress doesn't particularly want to get involved with regulating the drug industry for fear of pushing innovation and U.S. jobs to overseas markets, meaning insurers and PBMs operate at a disadvantage.
For the time being, Merck and Bristol's checkpoint inhibitors are more of a U.S. story than an EU story, so I don't see select EU countries playing hardball with Merck as necessarily a bad thing. However, as EU sales ramp up, we could begin to see some small level of gross margin degradation for companies like Merck. It's definitely something you'll want to keep your eyes on moving forward.