
Image source: Getty Images.
Somebody get the gurney, because Medicare is sick.
Ask seniors about their most immediate concern and you'll likely hear about the Social Security program's impending cash shortfall, which is forecasted to happen by the year 2034. But this same forecast from the Social Security and Medicare Board of Trustees is trumped by the fact that Medicare's Hospital Insurance Trust is expected to deplete its spare cash by the year 2028.
The Trustees' latest report noted that changing demographics had pushed the estimated depletion date earlier by two years from its 2015 report, which had predicted 2030. If this spare cash is exhausted and Congress does nothing, Medicare would become a budget-neutral program, paying out only the amount received via payroll taxes. The Trustees estimate that this'll lead to a 13% cut in reimbursements to physicians and hospitals.
What exactly do I mean by "changing demographics"? According to the Trustees' report, higher medical utilization rates and lower payroll tax revenue than initially projected have increased the estimated actuarial deficit of the program.
But there's more to Medicare's problems than just more seniors qualifying for coverage and visiting their doctors. The other issue is that medical care inflation, specifically as it relates to branded and specialty prescription drugs, has gotten completely out of hand.

Image source: Getty Images.
Prescription drug inflation is soaring
According to the Rx Price Watch Report released by the AARP in February, prescription drug costs for older Americans had risen 174% between 2005 and 2013 to $11,341 annually. This figure denotes the costs for branded, specialty, and generic drugs paid for by seniors all rolled up into one convenient figure. For comparison, in 2013 the median income for seniors was just $23,500, and Social Security beneficiaries were averaging an annual take home of just over $15,500 a year.
In other words, some seniors could be forking over a good portion of their annual income to cover their prescription drug costs during retirement -- and if Medicare isn't there to pick up a substantial portion of the cost of this medical care, seniors could really be in bad financial shape.

Image source: Gilead Sciences.
What's to blame for prescription drug inflation that's vastly outpacing wage growth and the national inflation rate? Obviously fingers can be pointed at certain new drugs that have entered the marketplace.
For example, Gilead Sciences' (GILD 0.01%) hepatitis C drugs Harvoni, Sovaldi, and Epclusa are extremely effective at ridding detectable traces of HCV in the body, as well as emptying pocketbooks. Even with substantive gross-to-net discounts, Gilead's game-changing HCV drugs cost a small fortune. On a wholesale level, standard 12-week courses of Epclusa, Sovaldi, and Harvoni run $74,760, $84,000, and $94,500, respectively. Since HCV is a disease that tends to build over many years and decades, it's seniors and pre-retirees that are most likely to be taking this medication.
However, it's not just new specialty medications that are to blame. Price hikes from long-existing medications are wreaking havoc on Medicare.
A study released in late April by the University of North Carolina at Chapel Hill showed that orally administered cancer drugs in 2014 were more than 500% more expensive than orally administered cancer drugs in 2000, when adjusted for medical inflation. Lead study author Stacie Dusetzina specifically highlighted Novartis' (NVS +0.51%) leukemia drug Gleevec, which increased in price by an average of 7.5% per year between 2001 and 2014.
All in all, Medicare Part D spending on prescription drugs is expected to total $88 billion in 2016, and this figure appears primed to rise at a quick rate in the coming years.
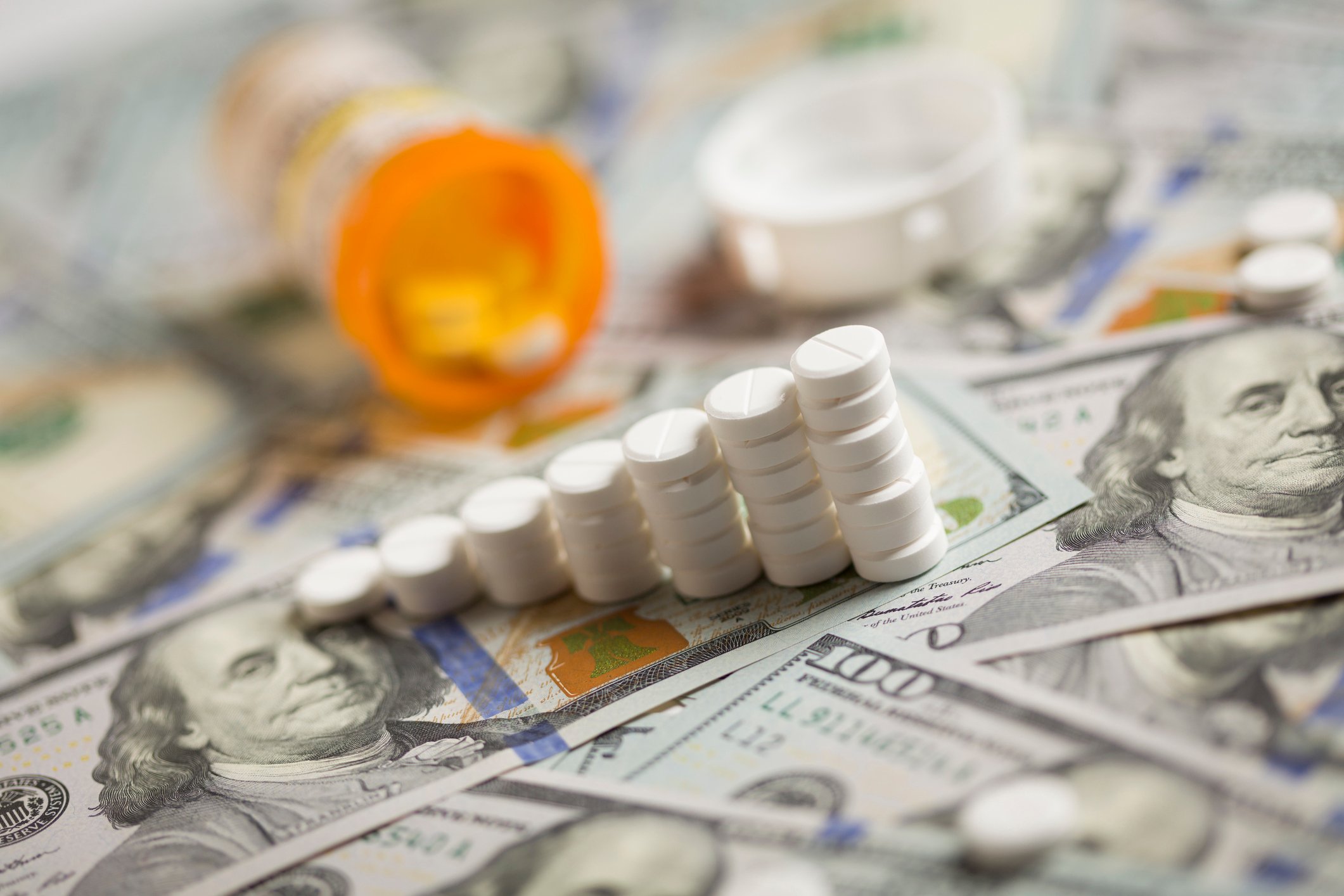
Image source: Getty Images.
Medicare could -- but isn't allowed to -- save at least $16 billion a year by doing this
Yet here's the kicker: Medicare could probably save billions of dollars -- at least $16 billion, if not more -- by doing one simple thing: negotiating its own drug prices with drugmakers.
Based on a study conducted by Carleton University and Public Citizen, Medicare could save $16 billion annually based on the $70 billion spent on prescription drugs in 2013. With the total prescription-drug spending figure rising to $88 billion this year, the assumption is the savings potential is much higher now, thus "at least $16 billion." Based on their research, Medicare is paying 83% of a brand-name drug's list price. Now compare this to Medicaid and the Veteran Health Administration, which pay 48% and 46% of branded-drug list prices according to the study.
The difference? Medicaid and the VHA are allowed to flex their negotiation muscles with drugmakers, which lands the two programs substantial gross-to-net discounts. Medicare, though, has its hands tied. The 2003 Medicare Modernization Act barred the program from directly bargaining with drugmakers, which instead leaves insurers to handle the hard work. Based on the data above, insurers aren't doing a very good job of going to bat for their members.

Image source: Getty Images.
The solution would seem pretty simple: allow the government to use its might to bargain for better drug prices for seniors. The resulting savings could help put extra money back into the pockets of seniors and the program. It's also a solution that a number of Americans favor, at least based on a 2015 Kaiser Family Foundation (KFF) poll. KFF's survey found that 83% of respondents favored government involvement if it meant lower prescription drug costs.
This solution is far from perfect
But there's a catch. Allowing government involvement would disrupt the free market that drug companies currently enjoy. Disrupting the free market is an idea that lawmakers on Capitol Hill may not appreciate, even if the American public overwhelmingly favors it.
Even more so, allowing the government to use its might to negotiate lower drug prices could drive jobs and innovation within the sector overseas. Lower margins could cause U.S. drugmakers and biotech companies to seek out more cost-competitive environments, costing U.S. jobs in the process. Let's not forget that domestic drugmakers count on the high margins and strong drug pricing power in the U.S. to subsidize their ventures into emerging and underdeveloped markets. If those high margins get reduced, innovation could suffer and emerging markets could see a reduced access to life-saving medicines.
There's no questioning that Medicare needs a fix, as the current path appears unsustainable. But exactly how lawmakers will fix Medicare remains to be seen.





